You’ve probably heard of gingivitis, or gum disease, from a million mouthwash ads. But you may not have heard of periodontitis.
Dentists diagnose and manage periodontitis based on well-established clinical guidelines and decades of research into how gum disease affects oral and overall health.
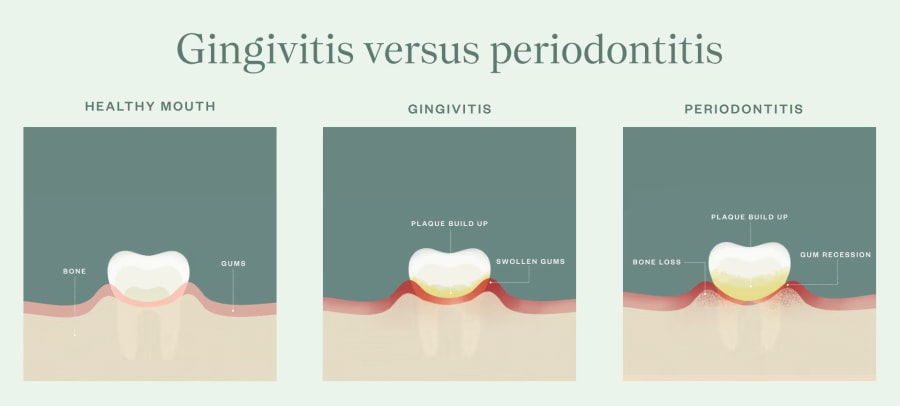
Think of the two as a progression. Plaque is a sticky film of bacteria that forms on teeth every day. When this buildup disrupts the balance of the oral microbiome, inflammation can develop along the gumline and lead to gums that are sensitive and inflamed. That’s called gingivitis, and it represents the early stages of gum disease. Some of the most common signs of gingivitis are bad breath and bleeding gums when you brush.
If gingivitis isn’t treated, your gum tissue can start to pull away from the structures that support it, and you may suffer bone loss. Ultimately, your teeth may loosen or fall out. That’s called periodontitis.
Periodontitis is a serious disease
Even though it affects almost half of American adults over 30, periodontitis isn’t something that should be taken lightly. It’s a serious condition that can lead to irreversible damage to the gums and bone that support your teeth, even though discomfort from the condition is often minimal. Advanced periodontitis (periodontitis that has progressed to its latest stages) can require invasive, costly surgical interventions like bone and soft tissue grafts.
Once it has developed, periodontitis can’t be cured, but it can be controlled through a combination of diligent at-home care and non-surgical periodontal treatment.
What causes periodontitis, and how it progresses
The short answer to what causes periodontal disease is plaque buildup, but how it progresses and how bad it ultimately gets really depends on how long inflammation is left untreated. Understanding how plaque affects your gum health can make the condition feel far less mysterious and far more manageable.
Stages of periodontal disease
Periodontal disease develops gradually, moving through clear stages when plaque and inflammation are left untreated. The earlier it is caught, the easier it is to manage and protect your smile.
Stage 1: Gingivitis
Gingivitis is the earliest and most reversible stage of gum disease. It begins when plaque, a sticky film of bacteria, builds up along the gumline. If plaque is not removed with daily brushing and flossing, it can harden into tartar, which requires a professional dental cleaning to remove.
When gingivitis takes hold, gums often look red, feel tender, or bleed when brushing or flossing. At this stage, inflammation is limited to the gums, and the bone that supports your teeth is still healthy. Learn more about early gum disease in our guide to gingivitis.
Stage 2: Early periodontitis
When gingivitis is left untreated, inflammation can cause the gums to pull slightly away from the teeth, forming small spaces called periodontal pockets. These pockets allow bacteria to collect below the gumline, where regular brushing cannot reach.
As these periodontal pathogens (bacteria) build up below the gumline, the body’s immune system works overtime to fight the infection, setting the stage for deeper inflammation. This is the point where gingivitis becomes periodontitis. Early tissue damage may begin, but timely care, including professional cleanings and personalized guidance, can help slow progression.
Stage 3: Moderate periodontitis
As pockets deepen, bacteria continue to build up beneath the gums. The body’s immune response stays activated, which can begin breaking down the bone and connective tissue that hold teeth in place. Ongoing inflammation like this is also linked to broader overall health risks, which is why managing gum disease matters beyond your smile.
Symptoms like gum recession, lingering bad breath, or changes in how teeth feel when chewing will become increasingly noticeable. At this stage, targeted periodontal care, such as non-surgical gum disease treatment, is often recommended.
Stage 4: Advanced periodontitis
Over time, without treatment, advanced periodontitis typically develops. Advanced periodontitis complications can include significant bone and tissue loss, loose or shifting teeth, and discomfort when chewing. Teeth may loosen, shift, or feel uncomfortable when chewing. Because much of the damage happens below the surface, symptoms may still be subtle until the disease is more advanced.
This is why routine dental visits and preventive care play such an important role in protecting long-term oral health and helping prevent periodontitis from progressing.
Risk factors that increase the likelihood of periodontitis
Plaque is the direct cause of periodontitis, but certain factors can make gum disease more likely to develop or progress. Having one or more risk factors does not mean you will develop periodontitis. It simply means your gums may need a little extra attention.
- Smoking and tobacco use: Tobacco reduces blood flow to the gums, slows healing, and weakens the body’s ability to fight infection. It can also hide early warning signs like bleeding.
- Diabetes: Poor blood sugar control increases inflammation and infection risk, while active gum disease can make diabetes harder to manage.
- Genetics: Some people are naturally more prone to gum disease, even with good oral hygiene. Family history matters.
- Dry mouth: Low saliva levels, often caused by medications or health conditions, allow bacteria to build up more easily.
- Oral hygiene habits: Inconsistent brushing and flossing let plaque harden into tartar, creating the conditions for gum disease.
- Stress: Chronic stress can weaken the immune system and contribute to habits that affect gum health.
- Hormonal changes: Pregnancy, puberty, and menopause can make gums more sensitive to plaque and inflammation.
- Systemic health conditions: Certain immune or inflammatory conditions can increase susceptibility to periodontal disease.
The encouraging news is that risk factors do not determine your outcome. With regular dental visits, personalized care, and consistent home habits, including daily flossing to help prevent gum disease, many people are able to protect their gums and slow disease progression.
Isn’t periodontitis a disease of older people?
Many people think periodontitis is a condition that only affects older adults, but that is a common misconception. While it is true that periodontal disease becomes more common with age, it can begin much earlier. According to the Centers for Disease Control and Prevention, about 70.1% of adults ages 65 and older have periodontal disease. At the same time, nearly half of U.S. adults over age 30, about 47.2%, already have periodontitis. This shows that gum disease is not limited to older adults and highlights the importance of early prevention and regular dental care.
How dentists diagnose periodontitis
Diagnosing periodontitis starts with a thorough dental exam. Your dentist will look for signs of gum inflammation, bleeding, and recession. To understand what’s happening below the gumline, they may gently measure the spaces between your teeth and gums to check for periodontal pockets and track changes over time.
Dental X-rays can be used to evaluate bone levels and spot damage that is not visible during an exam. If you are new to Tend, this process will be part of your first visit experience.
Together with your health history and risk factors, this information helps your care team understand the stage of gum disease and what your gums need next. From there, treatment can be tailored to your specific needs, with options designed to slow progression, promote healing, and protect your long-term oral health.
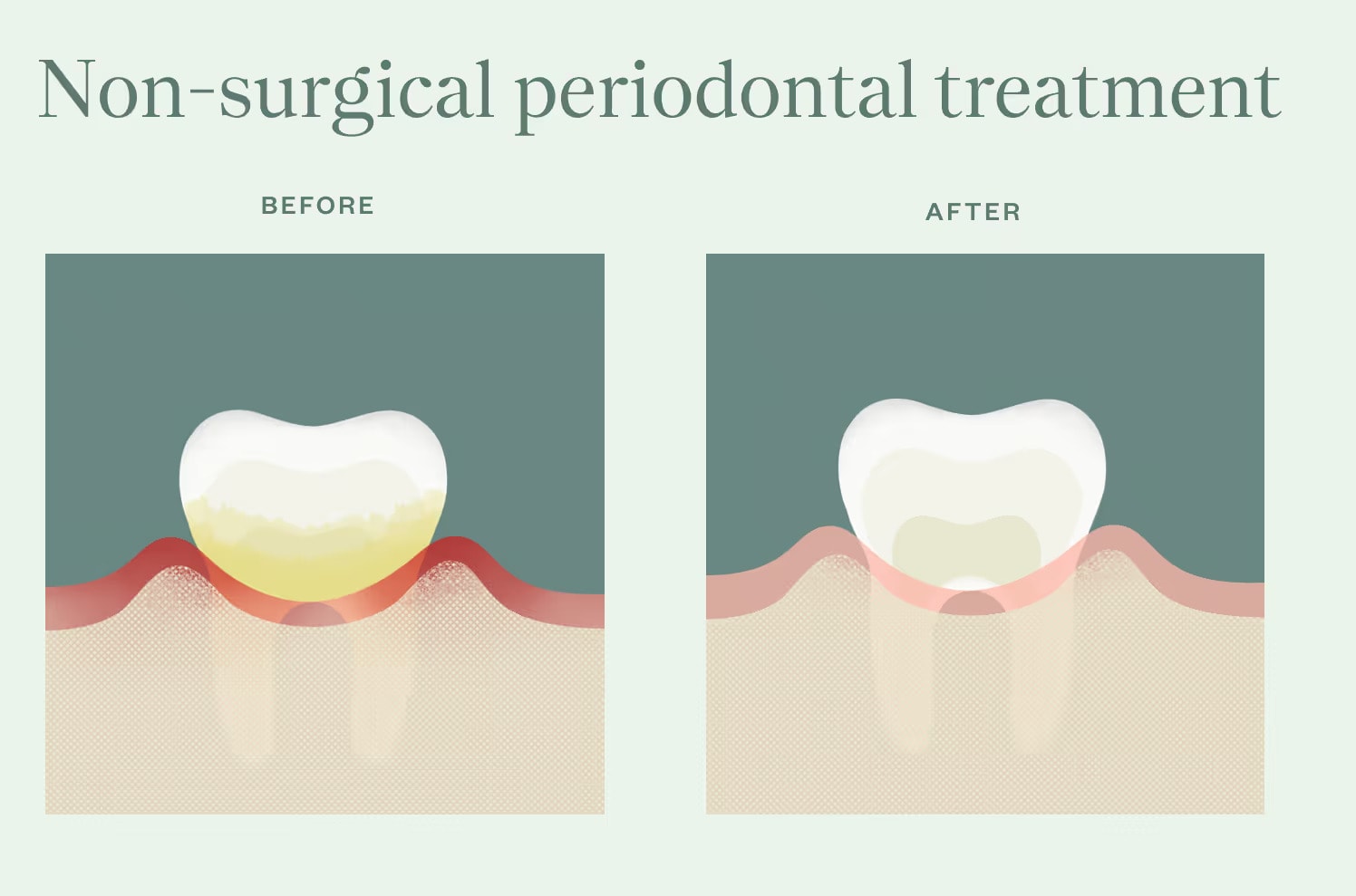
What is non-surgical periodontal treatment?
Non-surgical periodontal therapy is often the first step in treating periodontitis, and for many people, it is all that’s needed to get gum health back on track. The most common approach is scaling and root planing, a deep cleaning that targets bacteria below the gumline where everyday brushing and flossing can't reach.
How periodontal scaling and root planing work
Scaling and root planing focus on removing plaque and tartar hidden below the gums and along the tooth roots. Your dentist or hygienist will carefully clean these areas, then smooth the root surfaces to help the gums heal and reattach more comfortably around the teeth.
By clearing away the bacteria that cause inflammation, this treatment helps stop further tissue or bone damage by giving your gums the chance to calm down and heal.
Perio-Protect
In some cases, Perio Protect may be recommended as part of ongoing care. This at-home treatment uses custom trays to deliver medication directly into periodontal pockets, helping reduce harmful bacteria and promote healing between visits. It is often used alongside deep cleanings and regular maintenance to help keep gum disease under control long term.
What to expect during non-surgical periodontal treatment
Treatment is usually done in sections of the mouth, depending on how much care is needed. To keep you comfortable, a local anesthetic is typically used to numb the area being treated. Many patients are pleasantly surprised by how gentle the treatment feels.
Each appointment usually focuses on one section of the mouth and typically lasts about an hour, with treatment completed over a few visits. Your care team will explain each step ahead of time and help you understand the recommended timeline before getting started.
How long it takes to heal from non-surgical periodontal treatment
After treatment, some mild tenderness or sensitivity is normal for a few days. As healing begins, gums often feel less irritated, pockets may shrink, and gums can start fitting more snugly around the teeth again.
Most people return to normal routines right away, especially when following recommended home care, using proper brushing technique for gum health, and keeping up with regular dental cleanings.
Why non-surgical periodontal treatment is often the first step
Non-surgical periodontal therapy is considered the first line of treatment because it directly addresses the root cause of periodontitis: bacteria below the gumline. When caught early or treated promptly, scaling and root planing can slow progression and help preserve your natural teeth.
In some cases, deeper pockets or ongoing inflammation may require additional care. When that happens, your dentist will explain further options, including whether surgical periodontal treatment may be helpful, and guide you toward the treatment that offers your best chance at improved long-term oral health.
READ MORE: My Dentist Said I Can't Get A Normal Cleaning. Why?
How can I be sure I need this?
If you’re new to Tend Dental and your prior dentist never diagnosed you with periodontitis at any of your checkups, we know this may seem like a big deal over nothing. We want to assure you of two things.
First, Tend Dental practices evidence-based dentistry that’s rooted in the latest clinical research. We have an ethical duty to treat the medical issues we see, and we always adhere to the American Dental Association’s standards.
Second, our dentists don’t make a commission on procedures. They only present the treatment options you need. You can decide to proceed with any treatment recommendations, confident that your interests and your dentist’s are aligned.
Your dentist may also recommend specific at-home tools, such as floss, brushing adjustments, or a mouthwash for gum disease prevention, based on what will best support your gum health.
Periodontitis FAQs
-
Can brushing and flossing reverse periodontitis?
Brushing and flossing alone cannot reverse periodontitis, but they play a critical role in managing it. Once gum disease has progressed beyond gingivitis, professional treatment is needed to remove bacteria below the gumline.
That said, daily brushing and flossing are essential for preventing further damage, supporting healing after treatment, and reducing the risk of progression.
-
How is periodontitis different from gingivitis?
Gingivitis and periodontitis are related, but they are not the same condition. Gingivitis is the earliest stage of gum disease and involves inflammation of the gums caused by plaque buildup. At this stage, there is no bone loss and the condition is fully reversible with proper care.
Periodontitis develops when gingivitis is left untreated. Inflammation causes the gums to pull away from the teeth, forming periodontal pockets where bacteria can collect. Over time, this can lead to bone loss and damage to the structures that support the teeth.
-
How long does periodontal treatment take?
The length of periodontal treatment depends on the severity of the disease. Non-surgical periodontal treatment, such as scaling and root planing, is often completed over a few visits, with each appointment typically lasting about an hour per section of the mouth.
After initial treatment, ongoing maintenance visits help keep gum disease under control. Your dentist will recommend a timeline based on your individual needs and how your gums respond to care.
-
Is periodontitis curable?
Periodontitis is not curable, but it is manageable. Once bone and connective tissue loss occurs, that damage cannot be fully reversed. However, with professional treatment, consistent home care, and ongoing maintenance, periodontitis can be controlled and progression can be slowed or stopped.
Many people with periodontitis are able to keep their teeth healthy and functional for years with the right care plan.
-
What is the average age for periodontitis?
There is no single age when periodontitis begins, but it becomes more common as people get older. According to the Centers for Disease Control and Prevention, nearly half of U.S. adults over age 30 have periodontitis, and prevalence increases significantly after age 65.
That said, periodontitis can begin much earlier, especially in people with risk factors like smoking, diabetes, or inconsistent oral care. This is why regular dental visits are important at every age.
Periodontitis is a serious disease and needs to be treated
Take advantage of your dentist’s diagnosis to halt your disease before it advances, and restore your mouth to health.
Book Now